Pus is a protein-rich thick fluid that consists of living and dead white blood cells, dead tissues, plasma proteins, and bacteria.
- These are liquified products of inflammation resulting from bacterial, viral, or fungal infections to fight off infections.
- Pus oozes out from wounds or infected parts of the body. It’s also called purulent exudate, purulent drainage, or liquor puris.
- These are semifluid and viscous and form part of the innate immune response.
- The color of pus depends upon the location and type of infection. These are typically white, pale yellow, tinted green or brown, and opaque. The color of pus is a result of an accumulation of dead neutrophils.
- Sometimes, the green color of pus might be due to the production of green antibacterial proteins called myeloperoxidase by white blood cells.
- Moreover, Pseudomonas aeruginosa produces a green pigment known as pyocyanin. Similarly, yellow pus could indicate Staph infection or Strep, and brown pus of liver infection.
- Red tinges in pus can be seen when the blood seeps into the affected area.
- It’s odorless but may sometimes give a foul smell which could indicate a specific type of infection. For example, Pseudomonas aeruginosa infections, the common health-acquired infections, are particularly noxious.
Interesting Science Videos
Formation of Pus
The process of formation of pus is known as suppuration. It’s commonly caused by infection with pyogenic (pus-producing) bacteria, such as Staphylococcus, Gonococcus, Meningococcus, and Streptococcus.
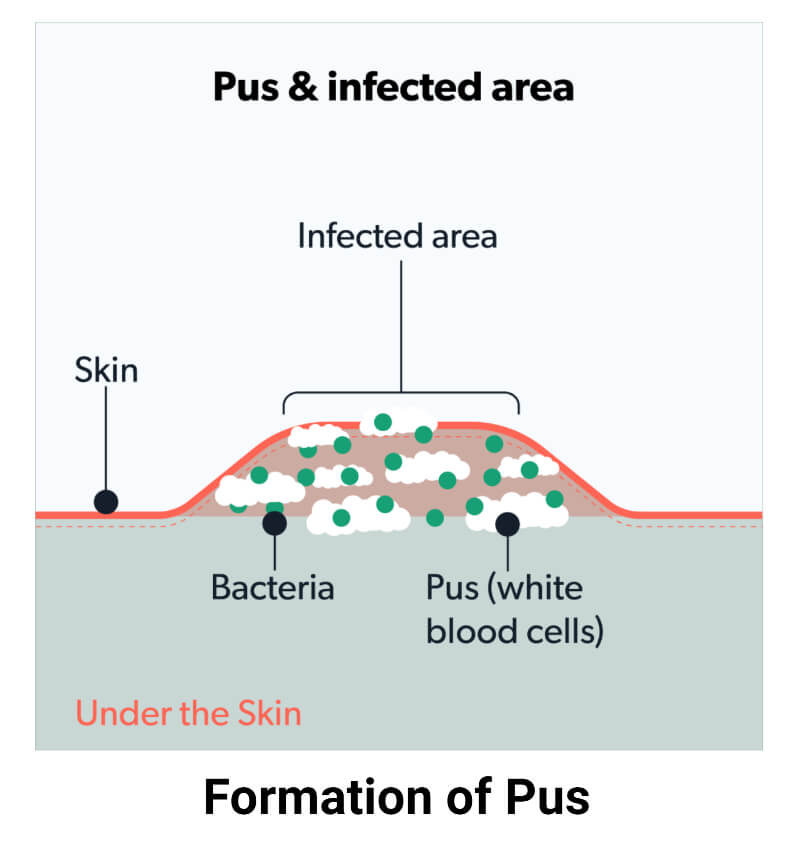
When pathogens invade our body, macrophages release cytokines which signal neutrophils to arrive at the site to fight the infection. The neutrophils release granules to combat the infection; likewise, bacteria secrete toxins known as leukocidins to make the counter-attack. Some neutrophils die because of either bacterial toxins or their inability to regenerate after releasing granules. Eventually, pus formation takes place.
Different types of pus-filled eruptions
Pustules or pimples are the accumulation of pus on or near the skin’s surface, and abscesses are filled with pus in the deeper tissue. Pus formation depends on the location of the infection.
Skin infection
Usually, in skin infections, the invading microorganisms are the ones that live on the skin (commensals), such as Staphylococcus aureus, methicillin-resistant S. aureus (MRSA), and Streptococcus pyogenes. These are opportunistic when finds cuts or abrasions find out their way inside the skin into deeper tissues and cause infections and pus formations. Pus-filled lesions that are visible and are red, raised, and painful fall under skin infections. These include:
- Acne: It is a condition where pores of the skin that open to hair follicles are blocked with oil, dead skin, or bacteria.
- Folliculitis: A skin condition where inflammation of one or more hair follicles is evident in a limited area.
- Boils or furuncles: A deep form of bacterial folliculitis is called a boil.
- Carbuncles: A carbuncle is a cluster of several boils connected.
- Superficial surgical site infection: Infection of the skin at the surgical site, which follows the pus formation along the incision, is a superficial surgical site infection.
Internal infection
Besides the skin, pus can be developed in our mouth, the root of an infected tooth, in the urinary tract, or around our tonsils. Moreover, severe purulent infections are associated with internal organs such as the lungs, spinal cord, or brain. Pus-filled abscesses are:
- Empyema: It is the condition where pus gets collected in the pleural cavity, i.e., the area between the lung and the inner surface of the chest wall.
- Brain abscess: The medical condition in which pus-filled pockets are found in the brain due to bacterial, viral, or fungal infections is called brain abscess.
- Septic arthritis: It is a bacterial, fungal, or viral infection in the joint fluid and joint tissues that spreads through the bloodstream into other parts of the body.
- Tooth abscess: A pocket of pus formed due to bacterial infection. A decayed or broken or injured tooth can result in a tooth abscess.
- Deep surgical site infection: The infection that occurs in the internal tissues and muscles beneath the incision area.
Significance of Pus
- The presence of pus is a good indicator of an actively functioning immune system.
- The poor or weakened immune system of an individual cannot produce enough white blood cells to combat infection resulting in serious, fatal, chronic, debilitating illnesses such as cancer and AIDS.
- The color, odor, and characters bolster the diagnosis. They help to direct in choosing suitable antibiotics, particularly when bacterial identification takes a longer period or during emergency conditions.
- These can be detrimental during the medication as antibiotics cannot penetrate a pocket of pus to digest the bacteria there.
Risk Factors for Pus Formation
Different factors likely to increase pus formation include:
- Severe trauma and burns
- Chronic alcohol intake
- IV drug use
- Chronic steroid therapy and chemotherapy
- Prolonged systemic illness
- Diabetes
- Immune disorders such as HIV, cancer, etc.
- Poor hygienic conditions
- Aging
- Nicotine addiction
- Delayed antibiotics treatment
- Obesity
- Unhygienic environment
- Sickle cell disease and Crohn’s disease
- Peripheral vascular disorders
Symptoms of Pus
Symptoms depend on the location of abscesses in the body. General symptoms of skin and internal infections include:
- High body temperature
- Pain and tenderness in the infected area
- Chills
- Redness and warmth in the affected area
- Discomfort in the abscessed area
- Excessive sweating
- Loss of appetite
- Weight loss
- Fatigue
- Swelling (edema)
Treatment of Pus
Pus treatment depends on the size and location of the affected area.
- Pus from small abscesses on the skin’s surface can be drained by applying a wet, warm compress a few times a day for several minutes.
- Seek medical help to draw out the pus from abscesses that are deeper, bigger, and difficult to reach.
- The therapies for pus treatment include antibiotics administration, drainage procedures, and other surgical treatments.
Prevention of Pus
- Hygienic lifestyles and practices such as avoiding smoking, balanced diet intake, doing exercises, washing hands regularly, etc. should be followed.
- All cuts and abrasions should be cleaned with soap and water, and apply an antibacterial ointment.
- The cuts and wounds should be bandaged, and the bandage should be changed frequently.
- Pus should not be squeezed out of pimples or boils.
- Towels, toothbrushes, or razors should not be shared.
References
- https://www.verywellhealth.com/what-to-do-about-pus-from-a-wound-or-incision-3157314
- https://www.medicalnewstoday.com/articles/249182
- https://www.singlecare.com/blog/what-is-pus/
- https://www.orlandosentinel.com/news/os-xpm-2001-03-11-0103110032-story.html
- https://www.webmd.com/a-to-z-guides/abscess
- https://www.nhs.uk/conditions/abscess/
- https://ro.co/health-guide/what-is-pus-and-treatment/
- https://factdr.com/health-conditions/pus/
