Microbe Notes is an educational niche blog/website related to microbiology (bacteriology, virology, parasitology, mycology, immunology, molecular biology, biochemistry, etc.) useful for biology and microbiology courses (High School, B.Sc, M.Sc., M.Phil., and Ph.D.).
Choose Notes Categories
Latest Notes
- Cholera: A-Level Biology Revision Notes
- Infectious Diseases: A-Level Biology Revision Notes
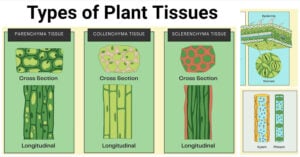
- Types of Plant Tissues: Meristematic and Permanent Tissue
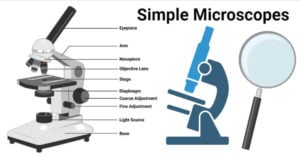
- Simple Microscope: Principle, Parts, Uses, Examples, Diagram
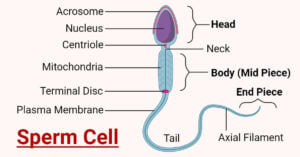
- Sperm Cell: Anatomy, Structure, Functions, Diseases
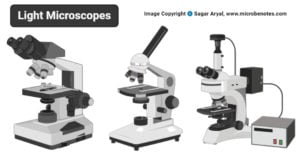
- Light Microscope: Principle, Types, Parts, Diagram
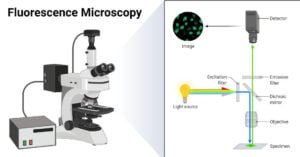
- Fluorescence Microscope: Principle, Parts, Uses, Examples
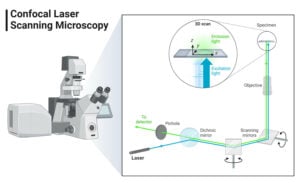
- Confocal Microscope: Principle, Parts, Types, Diagram, Uses
- Understanding Forest Ecology and Management
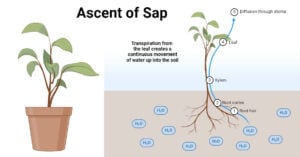
- Ascent of Sap: Definition, Mechanisms and Theories
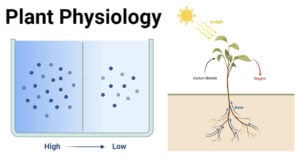
- Plant Physiology: Understanding the Life Processes of Plants
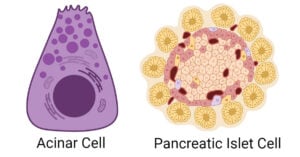
- Pancreatic Cells: Types, Structure, Functions, Diseases
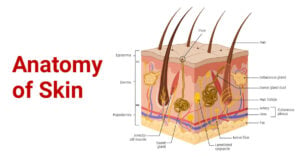
- Skin Cells: Structure, Types, Functions, Diseases
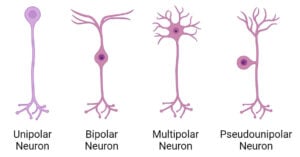
- Nerve Cells (Neurons): Types, Structure, Functions, Diseases
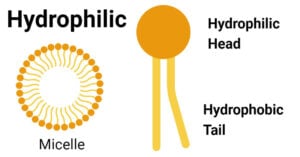
- Hydrophilic Molecule: Definition, Examples, Applications
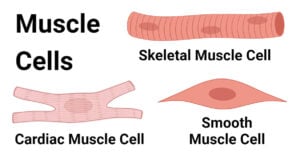
- Muscle Cells: Types, Structure, Functions, Diseases
- Compound Microscope: Principle, Parts, Uses, Diagram
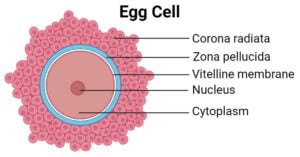
- Egg Cell: Structure, Types, Functions and Oogenesis
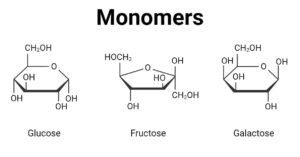
- Monomers: Types, Examples, Classification, Uses
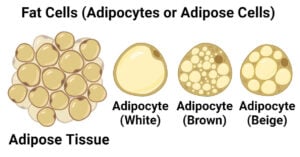
- Fat Cells: Definition, Types, Structure, Functions, Diseases